Medical Billing for Ambulatory Surgery Centers: A Complete Guide
Ambulatory surgery centers (ASCs) have transformed outpatient surgical care over the past three decades, delivering high-quality procedures at significantly lower costs than hospital outpatient departments. But the financial engine behind a successful ASC depends entirely on billing accuracy. Medical billing for ambulatory surgery centers is a specialized discipline that involves facility fee structures, implant pass-through billing, multiple procedure discounting rules, and payer-specific contract negotiations that differ substantially from traditional physician office billing.
Contact AMS Solutions for a free ASC billing assessment and discover how specialized billing expertise can maximize your surgery center’s revenue.
If your ASC is struggling with denied claims, underpayments, or lengthy accounts receivable cycles, the issue almost always traces back to billing complexity that demands specialized expertise. This guide breaks down the critical components of ASC billing so your team can identify gaps and make informed decisions about your revenue cycle.
How ASC Billing Differs from Physician Practice Billing
ASC billing operates under distinct fee schedules, coding requirements, and coverage rules that set it apart from standard physician practice billing. Many ASC administrators assume that billing processes used for physician practices translate directly to a surgery center environment. They do not, and the financial consequences of that assumption compound quickly.
The two primary billing streams within an ASC are:
- Facility billing: the ASC submits claims for the use of the facility, equipment, nursing staff, and routine supplies under its own National Provider Identifier (NPI).
- Physician billing: the operating surgeon, anesthesiologist, or other providers bill separately for their professional services under their own NPI.
This dual-billing structure means that coding errors or documentation gaps on either side can trigger claim denials, underpayments, or compliance exposure. Understanding how each element works, and how they interact, is the foundation of effective ASC medical billing.
For a deeper look at how Medicare and commercial payer coverage rules affect your claims, see AMS Solutions’ guide to navigating Medicare and Medicaid billing guidelines.
What Does ASC Facility Fee Billing Cover?
Facility fees are the cornerstone of ASC revenue. When Medicare or a commercial payer reimburses an ASC, the facility fee covers the overhead costs of performing a procedure: operating room time, nursing staff, disposable supplies, equipment depreciation, and routine drugs.
Medicare’s Ambulatory Payment Classifications (APCs)
Medicare reimburses ASC facility services using a payment system tied to Ambulatory Payment Classifications (APCs). Each covered procedure falls into an APC group, and Medicare pays a single packaged rate for that group. The ASC payment rate is set at approximately 57 to 60% of the Hospital Outpatient Prospective Payment System (HOPPS) rate, a built-in cost differential that makes proper documentation even more important for maximizing what you legitimately collect.
Key points for ASC facility fee billing under Medicare:
- Only procedures on Medicare’s ASC-covered surgical procedures list are reimbursable as facility services. Procedures not on this list must be carefully evaluated for site-of-service appropriateness.
- Packaged services such as anesthesia, most drugs, and certain supplies are bundled into the APC rate and cannot be billed separately.
- Correct procedure code selection and appropriate modifier usage are critical. Errors here create underpayments or outright denials.
- ASC Quality Reporting (ASCQR) program compliance affects payment; failure to report quality measures results in a 2.0 percentage point reduction in annual fee schedule updates.
Commercial Payer Facility Fee Contracts
Commercial insurers negotiate ASC facility fee rates directly with your center, typically as a percentage of billed charges, a percentage of Medicare rates, or a case rate. These contracts vary significantly by payer and by procedure type. Many ASCs are chronically underpaid simply because their billing team submits claims without verifying that the payment received actually matches the contracted rate.
Effective ASC billing requires a payment variance review process: every remittance should be checked against the applicable contract to catch underpayments before they become uncollectable write-offs.
How Are Implants Billed for ASC Procedures?
Implantable devices such as joint prostheses, spinal hardware, cardiac devices, and cochlear implants represent one of the most significant cost variables in outpatient surgery. For ASCs, recovering the actual cost of these implants is critical to financial viability, especially in orthopedic, spine, and cardiac cases.
Medicare Implant Pass-Through Rules
Under Medicare, certain high-cost implants qualify for “pass-through” status, meaning that the implant cost is paid separately from the standard APC facility fee rather than being bundled into it. Pass-through status is temporary (typically two to three years) and is intended to allow cost data to accumulate before the device cost is incorporated into the base APC rate.
To bill an implant pass-through correctly:
- Use the appropriate HCPCS pass-through device code (C-codes for hospital outpatient; transitional pass-through for ASCs has different qualifications).
- Document the device’s invoice cost; Medicare offsets the pass-through payment by any portion already included in the APC rate.
- Ensure your ASC’s cost report accurately reflects device acquisition costs.
Pass-through payments for devices are more limited for ASCs than for hospital outpatient departments. Many devices reimbursed as pass-throughs in the HOPPS system are simply bundled into the ASC rate without separate payment. Knowing which payers offer any form of implant carve-out, and negotiating this into your commercial contracts, is one of the highest-value billing and contracting strategies available to surgical centers.
Implant Billing for Commercial Payers
Commercial payer contracts vary widely on implant reimbursement. Some payers allow you to bill implants at invoice cost plus a markup percentage. Others apply a fee schedule rate regardless of actual cost. Many require prior authorization for high-cost devices and will deny the implant claim, or the entire case, if authorization was not secured in advance.
Best practices for implant billing include:
- Maintain an implant log documenting the device name, model, lot number, invoice cost, and implanting surgeon for every case.
- Review each payer’s implant policy before scheduling cases involving high-cost devices.
- Negotiate implant carve-outs or case rates that account for implant variability during contract renewals.
- Submit implant invoices with claims when required by payer policy.
Talk to AMS Solutions about maximizing your implant reimbursement recovery.
How Does Multiple Procedure Discounting Work in ASC Billing?
When two or more procedures are performed during the same surgical session, Medicare and most commercial payers apply multiple procedure discounting rules. Understanding how this works, and how to code it correctly, is one of the more nuanced aspects of ASC medical billing.
Medicare’s Multiple Procedure Rules for ASCs
Under Medicare’s ASC payment system, when multiple covered procedures are performed in the same operative session:
- The highest-valued procedure is paid at 100% of the applicable APC rate.
- Each additional procedure in a lower or equal APC group is paid at 50% of the full APC rate.
- Procedures with the same APC assignment are all paid at 50% after the first.
This discounting policy significantly affects reimbursement calculations when planning surgical scheduling and coding strategy. The sequencing of procedure codes on the claim form matters: place the highest-reimbursed procedure first. Swapping the order can inadvertently reduce payment when procedures share close APC values.
Bilateral Procedure Rules
Bilateral procedures add another layer. When the same procedure is performed on both sides of the body during the same session, Medicare typically pays 150% of the single procedure rate (rather than 200%). Use modifier -50 (bilateral procedure) correctly, and verify that your billing software applies this logic rather than doubling the standard rate, which would generate an overpayment and potential compliance exposure.
Add-On Codes and Bundling Edits
Medicare’s National Correct Coding Initiative (NCCI) edits and the Outpatient Code Editor (OCE) govern which procedure codes can be billed together and which are considered bundled. Unbundling, meaning billing separately for a component service that is part of a larger procedure code, is a compliance risk that can result in claim denials, audits, and overpayment demands.
Your billing team must regularly update their knowledge of NCCI edits and apply appropriate modifiers (such as modifier -59 for distinct procedural services) when two procedures are genuinely separate and distinct, documented in the operative report, and payable together under payer policy.
Common ASC Billing Challenges
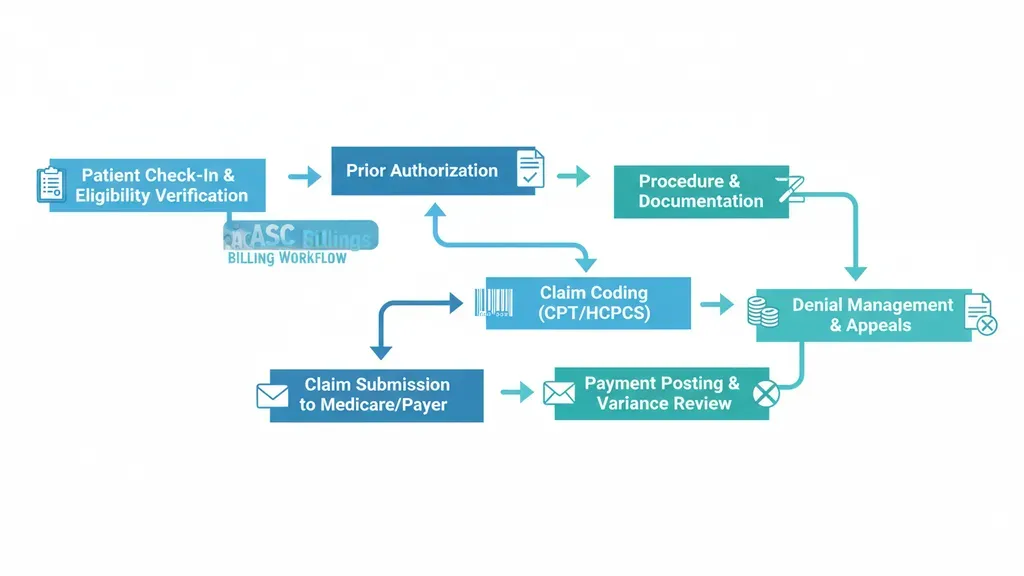
Even experienced ASC teams encounter billing obstacles that erode revenue. The most common issues include:
- Incomplete documentation: Operative reports that do not support the billed procedure codes, or that fail to distinguish between bilateral and unilateral services, are a leading cause of denials and downcoding.
- Authorization gaps: Failing to obtain prior authorization for procedures, implants, or out-of-network services creates denials that are difficult or impossible to reverse after the fact.
- Inaccurate patient eligibility verification: Verifying benefits before the procedure is performed prevents situations where the patient’s coverage does not include ASC facility services.
- Missed payer deadlines: Commercial payers have strict timely filing limits, often 90 days from the date of service. Claims submitted after the deadline are typically denied with no right of appeal.
- Incorrect modifier use: Missing or incorrect modifiers on high-complexity cases, bilateral procedures, and multiple surgeries cause systematic underpayments that compound over time.
- Credentialing lapses: If a surgeon or anesthesiologist performs a case before their credentialing with the relevant payer is complete, the facility claim may also be impacted. Keeping provider credentialing current is essential to uninterrupted billing.
- Accounts receivable aging: Without active medical accounts receivable management, denial backlogs and aging balances erode collections over time.
ASC vs. Hospital Outpatient: Key Billing Differences
| Factor | ASC Billing | Hospital Outpatient Billing |
|---|---|---|
| Fee Schedule | ASC-specific APC rates (57-60% of HOPPS) | Hospital Outpatient PPS (HOPPS) rates |
| Claim Form | CMS-1500 with ASC NPI | UB-04 (institutional claim) |
| Implant Pass-Through | Limited; most bundled into APC | Broader pass-through eligibility |
| Covered Procedures | Medicare-approved ASC procedure list only | Most outpatient procedures covered |
| Quality Reporting | ASCQR program (2% penalty for non-compliance) | OPPS quality reporting requirements |
Payer Contracting and Fee Schedule Optimization
Your ASC’s reimbursement potential is largely determined before a single claim is submitted. It is set by the fee schedules and contract terms you have negotiated with each payer. Many ASCs leave significant revenue on the table by accepting initial contract offers without negotiation or by failing to renegotiate as procedure volumes and costs evolve.
Areas to evaluate in your payer contracts:
- Are your rates pegged to a percentage of Medicare, and if so, is that percentage competitive with market rates in your region?
- Does the contract include carve-outs for high-cost implants or complex procedures?
- Are there escalator clauses that automatically adjust rates annually?
- What is the payer’s policy on implant billing, bilateral procedures, and multiple procedure discounting?
Bringing data to contract negotiations, using case mix reports, cost-per-procedure analysis, and denial rate breakdowns, gives your ASC leverage and demonstrates sophisticated financial management to payers.
Compliance and ASC Billing Integrity
ASCs operate under close scrutiny from Medicare, state regulators, and commercial payers. The Office of Inspector General (OIG) regularly includes ASC billing practices in its work plan, with particular attention to upcoding, implant billing, and unbundling. A robust compliance program that includes regular internal audits, staff training, and documentation review is not optional; it is a financial and legal necessity.
Key compliance safeguards for ASCs include:
- Regular coding audits comparing operative reports to billed procedure codes
- Annual review of NCCI edits and payment system updates
- Clear policies on medical necessity documentation for scheduled procedures
- Prompt self-reporting and repayment processes when billing errors are identified
Schedule a free compliance and billing review with AMS Solutions today.
Why Specialized ASC Billing Expertise Matters
The complexity of ASC billing, spanning facility fee structures, implant cost recovery, multiple procedure rules, and stringent compliance requirements, demands billing professionals who specialize in the surgical center environment. A generalist billing team, however skilled at physician practice billing, may lack the specific knowledge needed to optimize ASC revenue and maintain compliance.
Outsourcing your ASC’s medical billing to a dedicated revenue cycle partner delivers several advantages:
- Access to specialists who stay current with Medicare payment system updates, NCCI edits, and payer policy changes as their primary focus
- Systematic denial management and appeals, with every denial worked, not just the easy ones
- Payment variance reviews that catch payer underpayments before the appeal window closes
- Scalable capacity that accommodates procedure volume growth without proportional staffing increases
- Reduced internal overhead and elimination of staff turnover risk in a tight labor market for certified coders
For ASCs that also perform high volumes of orthopedic or musculoskeletal procedures, coordinating facility billing with your surgeons’ orthopedic medical billing ensures consistency and reduces the risk of conflicting claims.
How AMS Solutions Supports ASC Revenue Cycle Management
AMS Solutions has been delivering specialized medical billing and revenue cycle management services since 1986. Founded by physicians, we understand the operational and financial pressures that surgical facilities face. Our 100% U.S.-based team includes billing professionals with deep expertise in ASC facility billing, implant cost recovery, and complex surgical coding.
Our approach to ASC billing includes:
- Dedicated account representatives who know your center’s payer mix, procedure mix, and billing history
- Systematic claims scrubbing to catch coding and documentation issues before submission
- Active denial management and appeals with documented follow-up timelines
- Payment posting and variance analysis to identify payer underpayments
- Regular reporting so your leadership team has clear visibility into collection rates, denial trends, and A/R aging
We work with a wide range of surgical specialties and can integrate with your existing EHR and practice management software. There are no setup fees, no hidden costs, just a straightforward percentage-based fee tied to your collections.
Frequently Asked Questions About ASC Billing
What CPT codes are used for ASC facility billing?
ASC facility claims use the same CPT and HCPCS procedure codes as outpatient hospital claims. The distinction is in the bill type and the payer’s ASC-specific fee schedule. The claim is submitted on a CMS-1500 form (or electronically) using the ASC’s NPI and taxonomy code, not the physician’s.
Does Medicare cover all procedures performed at an ASC?
No. Medicare only reimburses ASC facility fees for procedures on its approved covered surgical procedures list. Procedures not on this list may still be performed at the ASC, but Medicare will not pay a facility fee; only the physician professional fee applies. Staying current with the annual updates to this list is an important part of ASC revenue planning.
How are anesthesia services billed for ASC cases?
Anesthesia professional fees are billed separately by the anesthesiologist or CRNA under their own NPI on a CMS-1500. The ASC facility claim does not include anesthesia professional services, though routine anesthesia supplies are packaged into the facility fee. If the anesthesia group is employed by or contracted with the ASC, revenue flow-through arrangements may affect how billing is structured.
How can an ASC reduce claim denials?
The most effective denial-reduction strategies include: thorough pre-authorization for all scheduled procedures and implants, accurate patient eligibility verification prior to the date of service, operative report documentation that clearly supports the billed procedure codes, and timely claims submission within each payer’s filing window. Partnering with an experienced billing team that actively manages denial trends is the single most impactful investment most ASCs can make.
Ready to Improve Your ASC’s Revenue Performance?
Medical billing for ambulatory surgery centers is too complex and too financially significant to leave to chance. Whether your center is struggling with implant reimbursement gaps, multiple procedure underpayments, or a growing A/R backlog, AMS Solutions has the specialized expertise to address the root causes and improve your collections.
We offer a free consultation and can provide a customized pricing quote in under 30 seconds. Contact our team today to learn how we can support your ASC’s revenue cycle, with no setup fees, no hidden costs, and billing professionals who work exclusively for you.
